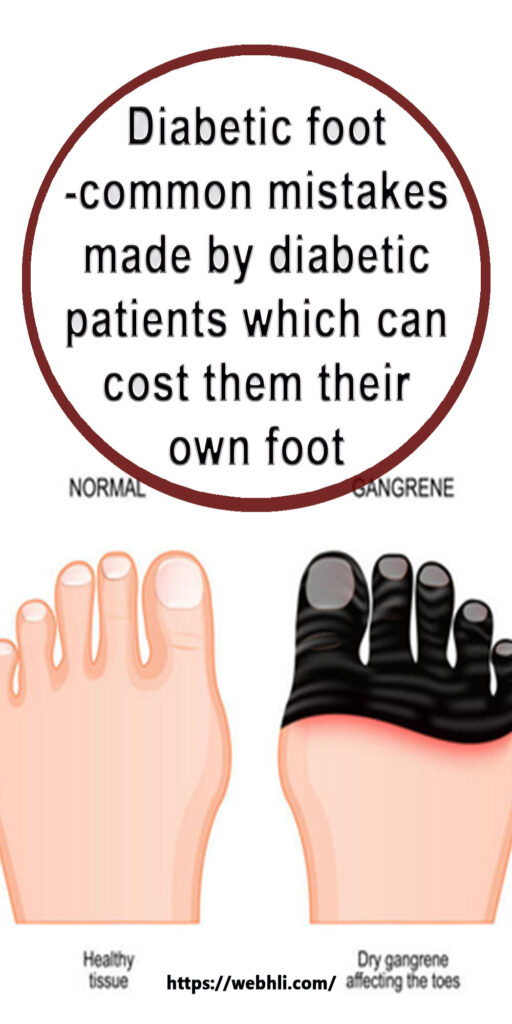
Diabetic foot|Podiatry -common mistakes made by diabetic patients which can cost them their own foot(essentials that every diabetic patients should know to avoid diabetic foot infections)
Prevention is the first step towards solving diabetic foot problems. It was estimated that every 30s, a leg is lost to diabetes somewhere in the world. A more important fact is that 85% of all amputations in diabetes are preventable.
Hence educating normal diabetic patients about the common reasons why they end up in amputation would make them take steps to avoid it when they encounter similar predisposing factors for diabetic foot infections
Diabetes affects the foot due to diabetic foot neuropathy or peripheral vascular disease(poor blood flow to foot)
Good Energy Food for Diabetics
10 Simple Food Concepts Every Person Living With Diabetes Should Know
Making Cheesecake For Diabetics
Enjoy the Taste and Benefits of Diabetic Foods
Will The Mulberry Leaf Help Your Diabetes?
5 DIABETIC FRIENDLY SALADS Some Tasty
DIABETIC LEMON COCONUT COOKIES Some Tasty
50 Healthy Diabetic Recipes That Are The Best
How does diabetic foot sensory neuropathy lead to infections?
It is loss of pain perception because of sensory neuropathy that catches many diabetic patients unaware of minor injuries(foreign bodies). The wound then gets infected. Hence, avoid walking barefoot since minor injuries are not noticed due to loss of pain percetion and walking with injury for several days, without any treatment leads to diabetic foot infections/amputations later.
How do shoes or footwear lead to diabetic foot problems?
Since the feet of diabetic patients swells in evening with neuropathy,a shoe that fits well in the morning may be too tight by end of day when feet swells,since perception of pain is lost in diabetic neuropathy patient continues to wear tight shoes for prolonged periods without comfort,end result would be blisters/infection at most compressed region by tight shoes
Those patients with loss of pain perception wear sandal with straps very tight for getting to know they are wearing footwear, these sometimes leads to compression for prolonged periods leading to blisters/infections
How does diabetic foot motor neuropathy lead to diabetic foot infections/amputations?
Motor neuropathy causes wasting of small muscles of foot leading to bony prominences and deformity formation like high arched foot,claw toes deformity etc,leading to high pressure at these localised bone deformity sites while walking .This lead to callus(hard skin) formation .In diabetic patients with sensory loss,if callus grows hard like stone they run the risk of developing an undetected wound underneath the callus.
How does callus lead to diabetic foot infections?
Callus has 11 fold increased risk of ulceration in diabetic patients with diabetic foot neuropathy,by using customized insole and outsole modifications according to individual needs can prevent further progression to ulceration
When does diabetic foot ulcer lead to infections?
Chronic diabetic foot ulcer/trophic ulcer not healing/not showing signs of improvement in wound size for more than 3 months has 15-20% chances of diabetic foot infection in their future.These are pressure ulcers that do not heal with routine dressing/antibiotics,these diabetic foot ulcers require footwear customization /podiatry surgeries if not resolving with footwear customization.Since 85% of amputations are preceded by poorly treated previous foot ulcer, best is to consult your foot doctor/podiatrist
How does diabetic autonomic neuropathy leads to diabetic foot infections?
Autonomic neuropathy leads to decreased functioning of sweat glands, in turn leading to loss of sweating and dry skin
Dry skin precipitates cracks/deep fissures with hard edges in sensory loss patients can lead to skin breakage and diabetic foot infections most commonly in heels,application of moisturizing cream /lotion can solve this problem
Dry skin precipitates itching sensation scratching too much can lead to skin breakage because of loss of pain perception diabetics will scratch till skin is breaking and sometimes cellulitis infections can occur when immunity level is low after long years of diabetes,application of moisturizing cream /lotion can solve this problem
Some patients complain of itching and persisting cracks even after applying moisturizing creams, why so?
It suggests that skin is becoming dry very often in these patients.Applying once a day will not solve the problem,They must increase the frequency of application to three to four times a day
Which foot swelling should be immediately treated?
Any abnormal unilateral foot swelling should raise suspicion of either charcot foot/quiecent bone infection/cellulitis foot,
Any unilateral foot swelling with redness in skin ,increased warmth over swelling,pain over swelling,skin discoloration over swelling should be consulted with your foot doctor for emergency treatment
How can self treatment in diabetic neuropathic pain land up in diabetic foot infections?
Patients with neuropathic pain try to do vigorous massage with ayurvedic oils/linments till skin blister formation because of loss of pain perception in sensory neuropathy
Other modality patient adopts in neuropathic pain is hot water massaging with sensory loss, patients do not know how much heat should be applied so they continue to keep very hot water for prolonged periods at pain areas leading to blister and diabetic foot infections
What causes interdigital fungal infection ?
Crowdy toes or tight shoes that keep toes tight retain moisture for prolonged periods and cause fungal infection,which could be avoided by using shoes with wide toe box/using toe separator to keep toes separated to prevent moisture retaining in between toes
Self surgery what can happen?
Patients with poor vision cutting nails too deep beneath crease line can lead to skin breakage and in patients with poor blood flow to foot can lead to major amputation.Proper nail cutting techniques should be learnt,toe nails should be cut straight,not beneath creaseline.
Patients with callus try to remove it with blades by themselves sometimes leading to skin cuts in adjacent areas and diabetic foot infections later.Always approach a foot doctor for callus trimming in diabetes
Are previous amputees at risk of future diabetic foot ulceration/infection?
Yes,biomechanics is altered in previous amputees so pressure points increase at other areas leading to callus/diabetic foot ulcer later diabetic foot infections,these could be avoided by proper customized footwear or proper surgical principle applied during time of amputation to prevent future pressure points.These are done by specialist diabetic foot surgeons.
Can we use oils instead of moisturing cream in foot and leg?
Sometimes due to fragnance of oil insects/ants are attracted,so there is a possibility of insect bite injury which again precipitates itching and scratching, finally skin breakage and sometimes diabetic foot infection
Check out these related articles, too:
What You Should Look Out For For Kidney Failure Symptoms?
Kidney Failure Treatment Without Dialysis
Kidney Diet Secrets That Can Reverse Chronic Kidney Failure
The Effects of High Potassium For Kidney
What Is A Healthy Kidney Diet Plan
Diet Tips For People With Diabetes and Kidney Disease
Are Renal Insufficiency And Kidney Failure The Same Thing
5 Natural Supplements For Chronic Kidney Disease
Bitter Melon Recipe For Diabetes
How does ingrown nail form and when can it lead to diabetic foot infection?
Because of improper nail cutting techniques like cutting nails at corners allows nail to grow deep inwards when it regrows,when ingrown nail is pressing skin for prolonged periods can compromise blood flow to adjacent skin leading to diabetic foot infection,these things could be avoided by learning proper nail cutting techniques
Diabetic patients may notice new small cuts in foot/toes when they wake up from bed, What could be the reason?Rat bite injury is common during night because it crawls in night and bite and since pain perception is lost in diabetic neuropathy patients does not move to rat bite which makes the rat to do the same on repeated nights present with newer cuts day by day
Source: Free Guest Posting Articles from ArticlesFactory.com


 Protected by Patchstack
Protected by Patchstack